Trusted by 500+ Healthcare Providers
Save upto 20% with Our Medical Billing Services
Clarte RCM helps you save thousands each year with specialty experienced billers and coders. We reduce denials, prevent compliance penalties, and lower AR days with 95% claim accuracy.
Get the Best Medical Billing Services in USA at Just 2.95%

Our Services
Clean Claim Scrubbing
See exaPre-submission checks for eligibility, NPI, taxonomy, modifiers, and payer rules.ctly what's happening on every screen.
Eligibility and Prior Auth Controls
270/271 checks and prior auth matching to prevent coverage-related denials.
Remittance Posting and Underpayment Review
Accurate CO and PR posting to catch underpayments and prevent write offs.

ICD-10-CM and CPT/HCPCS Coding Accuracy
Specialty coding with correct code selection, units, and sequencing.
Modifier and NCCI Edit Compliance
Proper modifier use with NCCI PTP checks to prevent bundling denials.
Documentation Review and Audit Support
Chart review to close gaps, support medical necessity, and reduce audit risk.

A/R Follow-Up and Timely Filing Control
Workqueues to prevent aging and protect filing and appeal deadlines.
Denial Root-Cause and Appeals Management
Reason-code triage, corrected resubmissions, and payer-ready appeals.
Payment Variance and Underpayment Recovery
Contract checks to spot underpayments and recover missed reimbursement.

Payer Enrollment and Contracting
Commercial, Medicare, Medicaid, and Blue Cross Blue Shield enrollment support.
CAQH and Provider Profile Management
CAQH upkeep with NPI, taxonomy, licenses, and attestations.
Recredentialing and Status Tracking
Deadline tracking and payer follow-up to prevent terminations and claim holds.

Chart-to-Claim Audit Review
Verify coding, modifiers, and documentation match billed services.
Denial and Edit Pattern Analysis
Identify trends in payer edits, NCCI issues, and recurring denial reasons.
Payment Accuracy and Variance Audits
Check allowed amounts, adjustments, & underpayments against contract terms.
Who We Serve
We offer customized medical billing services in the USA for all sizes and specialty practices.
Physicians
Hospitals
Healthcare Groups
Specialty Practices
Clinics
Clarte RCM Beats All Billing Challenges
If denials, claim rejections, and AR ageing are slowing your cash flow, we have experts to help.
Challenges
Billing issues usually start with small data and coding mismatches that trigger payer edits and slow payment. These gaps turn into rejections, denials, and aging AR. Challenges providers normally face are:
- Wrong payer plan or subscriber ID routes claims incorrectly
- Eligibility checked for the wrong date of service
- NPI and taxonomy mismatches with payer enrollment
- Prior auth approved but claim details do not match
- Modifier errors trigger NCCI PTP bundling denials
- Units exceed MUE limits and reject claim lines
- 837 format errors and missed TA1 999 277CA rejects
- CO and PR posting mistakes causing missed underpayments
Solutions
Our insurance billing services run a controlled workflow that prevents errors before submission and fixes issues fast after payer response. Our medical billing teams follow payer rules and keep every step aligned. Outsource billing services to us and ensure:
- 270 271 eligibility verification and plan validation
- Auth to claim matching for codes, units, dates and NPI
- Specialty coding checks for ICD-10-CM, CPT, HCPCS and modifiers
- NCCI PTP and MUE edits applied before claim build
- Provider data governance for NPI taxonomy POS and enrollments
- EDI monitoring for acknowledgments and rapid reject correction
- Denial workqueues based on reason codes with daily follow up
- Timely filing and appeal deadline tracking to protect recovery
- Payment posting with CO PR accuracy and variance review
Positive Outcomes
When your billing workflow is controlled, claims move faster, and your AR stays accurate. You see fewer delays, fewer write offs, and clearer reporting for better decisions. With our medical billing agency you achieve:
- Higher first pass claim acceptance
- Fewer denials from coding and payer edits
- Fewer clearing house and payer rejects
- Lower A R days and less aging
- Faster denial recovery and fewer write offs
- More accurate patient balances and statements
- Stronger compliance and audit readiness
- Underpayments caught and recovered earlier
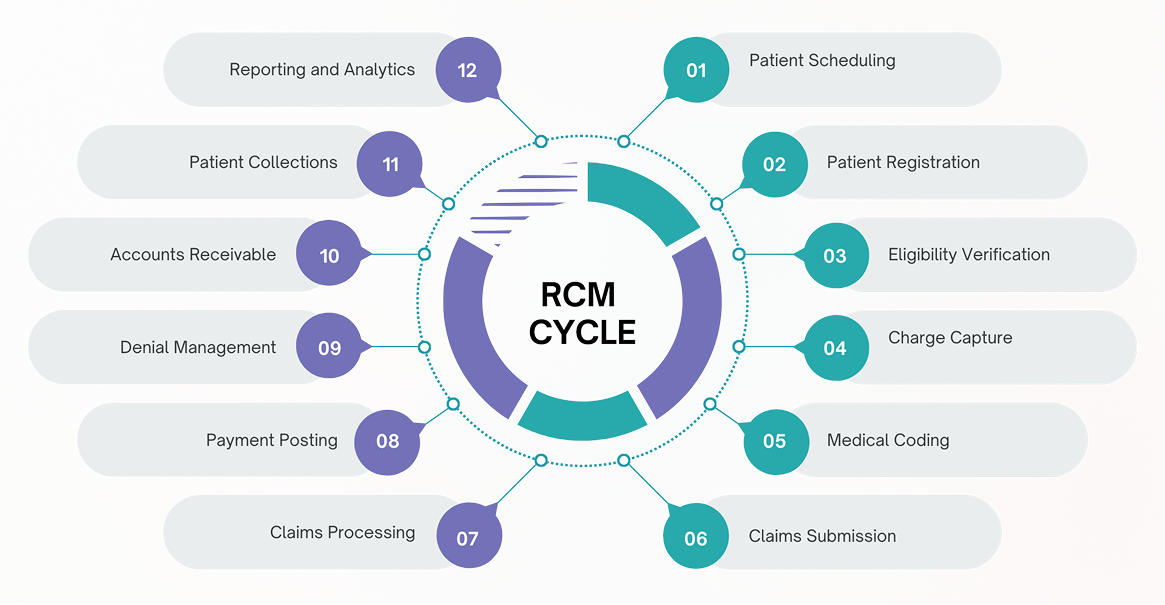
How Our Revenue Cycle Management Process Works?
Whether you want to outsource complete RCM or specific medical billing services, we offer both fully managed and customized support that fits your practice needs.
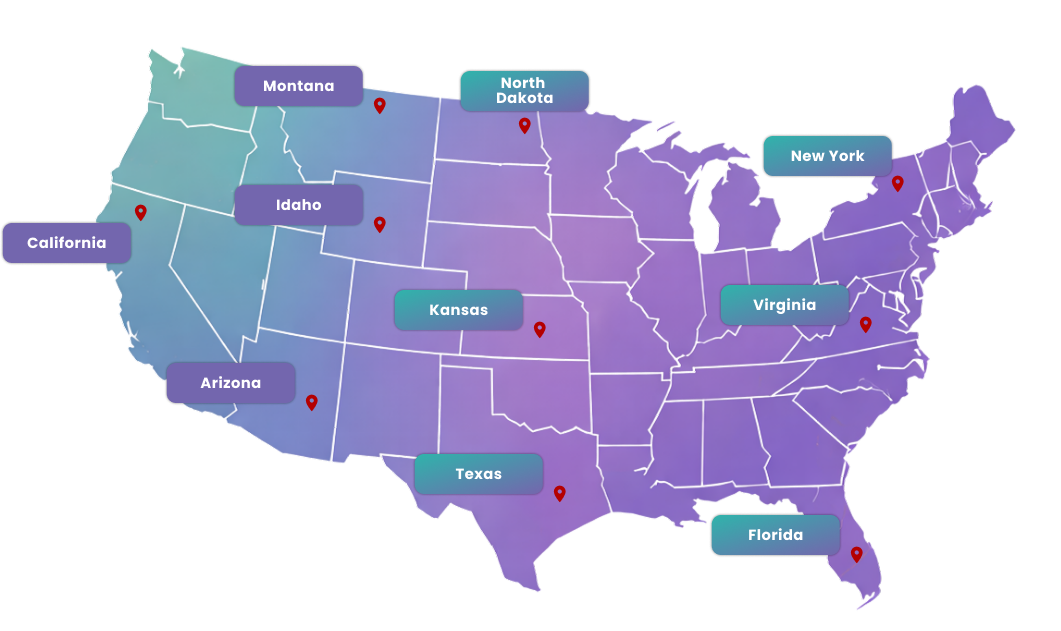
Medical Billing Services for All 50 States
We understand that billing laws and payer rules vary by state, so our medical billing company assign state-specific billing experts to keep your claims accurate and compliant.
Medical Billing Services for All Specialties
Internal Medicine
Nephrology
Family Practice
Wound Care
ASC
Urgent Care
Pulmonology
Cardiology
Behavioral Health
Dentistry
WHY CHOOSE US
Why Practices Recommend Clarte RCM
We reduce denials, lower AR days, and keep reimbursements steady.
Specialty Trained Billers
Billers and coders matched to your specialty & payer rules.
Clean Claim Controls
Eligibility and claim edits checked before submission.
AI Denial Recovery
Reason code triage, appeals, and daily payer follow up.
Accurate Posting
Correct CO and PR posting for clean balances.
Clear Reporting
Weekly updates on claims, denials, and AR.
Our Billing Services Are
Compatible with 600+ EHR/EMR/PMS Platforms
CareCloud
drchrono
CureMD
eClinicalWorks
Practice Fusion
Kareo
athenaHealth
RXNT
CareCloud
drchrono
CureMD
eClinicalWorks
Practice Fusion
Kareo
athenaHealth
RXNT
What Our Clients Say
Trusted by healthcare providers across the nation.
Dr. Daniel Park
Orthopedic Clinic, TX
Michael Torres
Practice Manager, CA
Dr. Sarah
Family Medicine Practice, FL
Get expert claims billing services for better cash flow.
Frequently Asked Questions
What medical billing services do you offer?
Our medical billing company provides eligibility checks, charge entry, coding support, claim scrubbing and submission, denial management and appeals, payment posting, AR follow up, patient statements, reporting, and provider credentialing with dedicated accounts managers.
Do you offer medical billing services for small practices?
Yes. our medical billing company tailor workflows for small medical practices, handle claims and follow ups, and provide clear reporting without adding overhead to your team ith our CPB and RHIA certified medical billers.
How quickly can you take over billing without disrupting our cash flow?
We use a controlled onboarding process with EHR access setup, claim testing, and a staged go live so billing continues without gaps.
How is pricing calculated for your clinical billing services?
Pricing is based on your monthly claim volume, specialty complexity, payer mix, and the level of service you need, such as billing only or full RCM. Our medical billing service provider share clear pricing upfront with no hidden charges.
Why Work with us?
- Under 1% Rejections
- 99% Claim Acceptance
- HIPAA Compliant Workflow
- Pricing From 2.95% of Collections
- Practice Billing Audits
- Stronger Cash Flow, Fewer Errors

